SOSORT 2024 : presented studies, news and comments
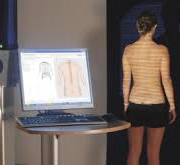
“This 2024 edition of the annual SOSORT conference, held in Boston, was also an opportunity for discussion, involvement, and growth. Every year, the level of research presented at SOSORT continues to rise, and we at ISICO are always at the forefront, commented Professor Stefano Negrini, Scientific Director of our Institute. SOSORT is undoubtedly the congress that brings together the most important specialists and the most significant research at an international level on the rehabilitation treatment of scoliosis. There was lots of news and great satisfaction for our specialists, who enlivened the conference with nine research projects presented both with posters and oral presentations. Dr. Fabio Zaina presented a study on the ability of the ODI and the SRS 22 to distinguish adult patients with or without scoliosis. At the moment, neither of the two questionnaires is able to make the distinction; in the ODI, subjects with scoliosis have greater difficulty lifting weights and standing compared to those who don’t have it, but the difference is not significant. Our physiotherapy director, Michele Romano, led two ongoing studies on curves; instead, our physiotherapist, Alessandra Negrini, in addition to animating the pre-conference by talking about Telemedicine, presented a review study on sagittal measurements among healthy children and adults, up to 40 years of age, to collect and, if possible, arrive at an average overall data measurement of kyphosis, lordosis, and other sagittal parameters.
“I myself presented two studies on adherence to brace treatment measured with sensors: one is a review study that demonstrated that both the use of sensors and counselling, i.e., the support given to patients during the course of treatment, can increase adherence to therapy, while the second study identified sex and age as the main variables that influence patient compliance,” explains Prof. Negrini.
There are also three posters signed by ISICO. Dr. Greta Jurenaite has prepared a poster on a case report of patients with lumbar Scheuermann, which demonstrates that exercises and a corset can effectively treat the pain caused by this pathology and that the brace also improves spinal growth by reducing the deformity. Dr. Giulia Fregna instead presented a review in the field of trunk neurophysiology in a poster; finally, the European Prepare project was also discussed with a poster by Dr. Carlotte Kiekens, already present at other SOSORT conferences but at her first as an ISICO specialist with her own research. “The congress was really interesting and informative! We were pleased to note that the PREPARE poster attracted a lot of attention – comments Dr. Kiekens – I was surprised that many professionals still do not have a clear understanding of the fact that rehabilitation treatment requires a multi-professional approach, involving the patient in a collaborative process and including diverse components such as brace therapy, exercises, cognitive behavioural therapy (CBT), psychological support, education, and much more. ISICO stands out for its advanced approach in this field.”. As introduced by Dr. Kiekens, there has been much discussion about artificial intelligence and its applications in the assessment of scoliosis, the development of therapeutic strategies, and the prediction of treatment outcomes, added Professor Negrini. Our participation in the PREPARE project positions us at the forefront of these new applications, thanks to our constant commitment to research, which is fundamental for the improvement of therapies. To the specialists present in Boston, we must add those who worked on this research, from therapists Bruno Lionelli, Serena Quaggio, and Sara Rossi Raccagni to Dr. Giulia Fregna. Finally, a moment from the conference that we are pleased to share: the appointment of Dr. Sabrina Donzelli, part of the ISICO staff for many years, as SOSORT president for the next two years. The first woman in the history of this society: congratulations to Dr. Donzelli, a great professional.
We look forward to seeing you again at SOSORT 2025 in Dubrovnik!